
Medically Reviewed by Dr. Igor I. Bussel, MD
Board-Certified Physician | Last updated January 2026
Understanding Your Treatment Options
Obstructive Sleep Apnea (OSA) affects over 22 million Americans, causing repeated breathing interruptions during sleep. While CPAP (Continuous Positive Airway Pressure) therapy remains the gold standard first-line treatment, roughly half of patients struggle to use it consistently. For these individuals, surgical options offer a potential path to better sleep without nightly equipment.
CPAP Therapy: The First-Line Treatment
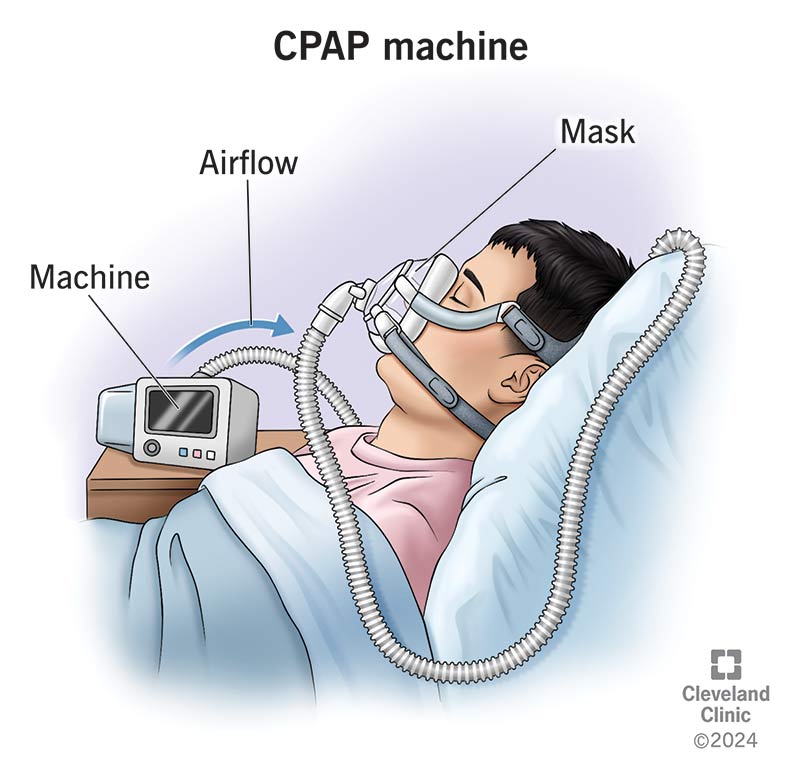
How CPAP Works
A CPAP machine delivers a constant flow of pressurized air through a mask worn during sleep. This air pressure keeps your airway open, preventing the collapses that cause apnea events. There are several variations:
- •CPAP: Delivers constant pressure throughout the night
- •APAP: Automatically adjusts pressure based on breathing patterns
- •BiPAP: Uses different pressures for inhaling and exhaling
Pros of CPAP
- ✓ Highly effective when used consistently
- ✓ Non-invasive - no surgery required
- ✓ Reversible - stop anytime
- ✓ Covered by most insurance plans
- ✓ Immediate symptom relief
Cons of CPAP
- ✗ ~50% of patients stop using within 1 year
- ✗ Mask discomfort and claustrophobia
- ✗ Dry mouth, nasal congestion
- ✗ Noise can disturb bed partners
- ✗ Requires nightly use for life
- ✗ Difficult for travel
Surgical Alternatives for Sleep Apnea
Surgery is typically considered when CPAP therapy fails or isn't tolerated. The goal is to physically address the anatomical causes of airway obstruction, potentially eliminating the need for nightly equipment.
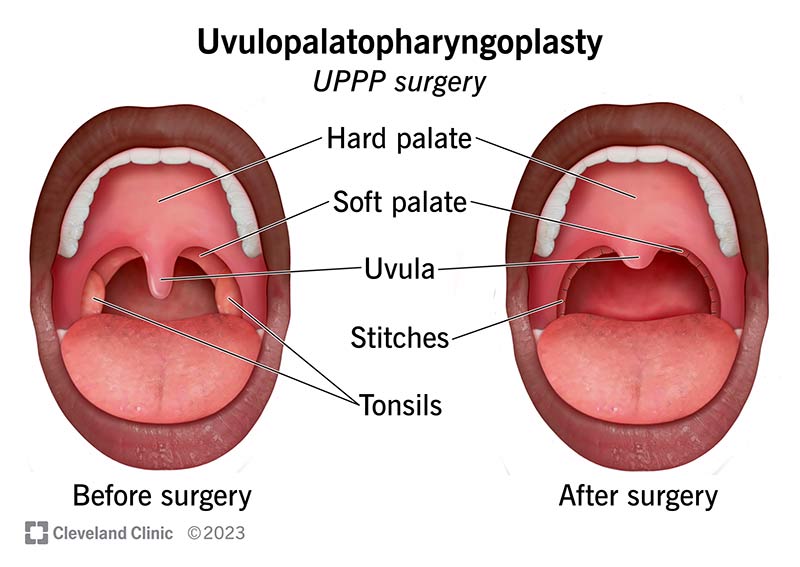
UPPP (Uvulopalatopharyngoplasty)
Removes excess tissue from the soft palate, uvula, and pharynx to widen the airway.
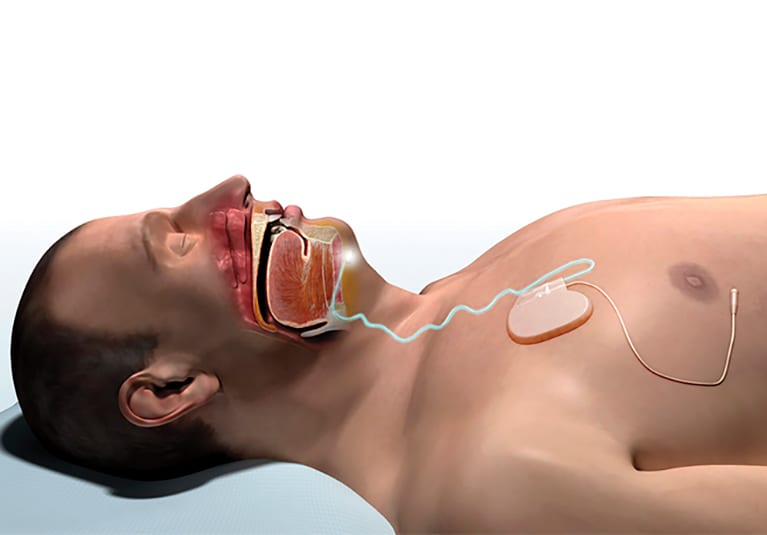
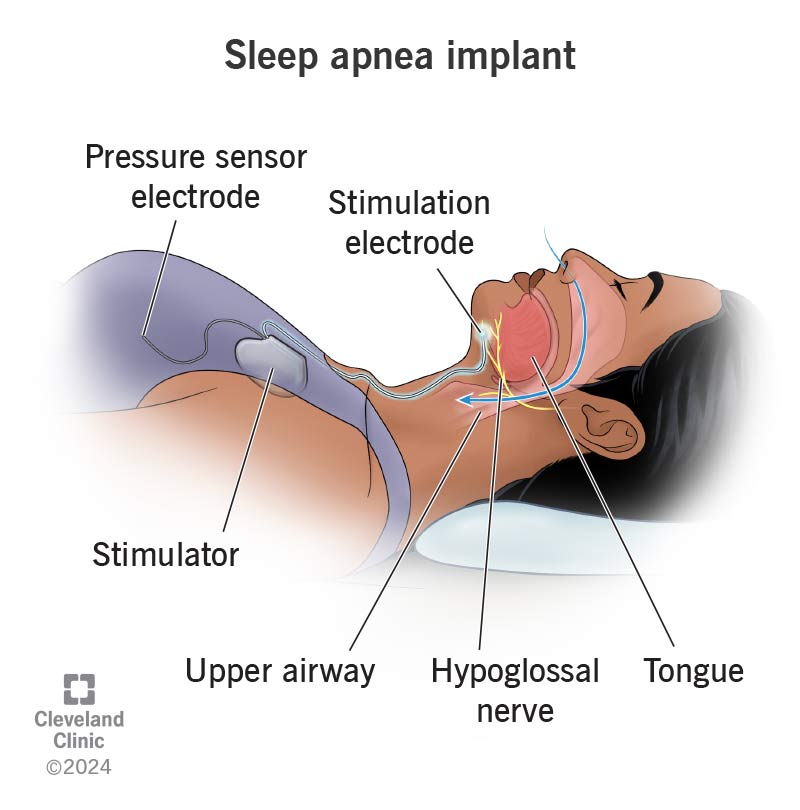
Inspire Therapy (Hypoglossal Nerve Stimulation) Most Popular
Implantable device stimulates the tongue nerve to keep the airway open during sleep.
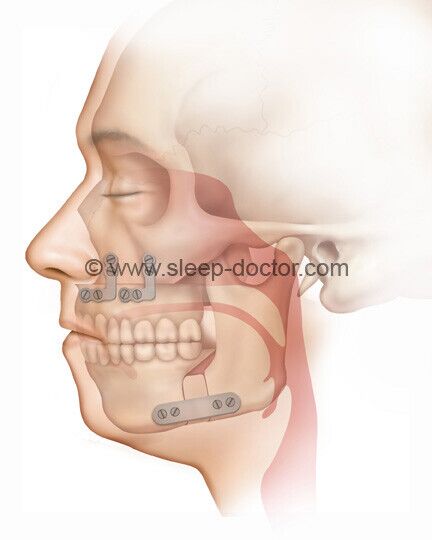
MMA (Maxillomandibular Advancement)
Repositions the upper and lower jaws forward to permanently enlarge the airway.
Pros of Surgery
- ✓ Potential for permanent solution
- ✓ No nightly equipment required
- ✓ Can be life-changing for right candidates
- ✓ Multiple procedure options available
Cons of Surgery
- ✗ Invasive with surgical risks
- ✗ Recovery time required
- ✗ Not guaranteed to cure OSA
- ✗ Higher upfront costs
- ✗ May need multiple procedures
Head-to-Head Comparison
| Feature | CPAP Therapy | Surgical Intervention |
|---|---|---|
| Invasiveness | Non-invasive | Minimally to highly invasive |
| Efficacy | High (with compliance) | 50-90% depending on procedure |
| Long-Term Solution | Requires nightly use | Potentially permanent |
| Common Side Effects | Mask discomfort, dry mouth | Pain, swelling, recovery time |
| Typical Cost | $500-$3,000 + supplies | $6,000-$100,000+ |
| Best For | All severity levels, first-line | CPAP-intolerant, specific anatomy |
Making Your Decision
Consider CPAP if:
- • You've never tried CPAP before
- • You prefer non-invasive treatment
- • You want immediate symptom relief
- • You have mild to moderate OSA
Consider Surgery if:
- • You've tried CPAP for 3+ months without success
- • You can't tolerate CPAP due to claustrophobia or discomfort
- • You have anatomical issues (enlarged tonsils, deviated septum)
- • You want a potentially permanent solution
- • Your lifestyle makes CPAP impractical (frequent travel)
Frequently Asked Questions
What is the success rate of sleep apnea surgery compared to CPAP?
CPAP is nearly 100% effective when used correctly, but compliance rates are around 50%. Surgery success varies by procedure: UPPP (40-60%), Inspire (79% AHI reduction), MMA (80-90%). The "best" option depends on individual factors.
If I fail CPAP, am I automatically a candidate for surgery?
Not automatically. You'll need a thorough evaluation including DISE (Drug-Induced Sleep Endoscopy) to determine the location of your airway obstruction. Some patients may benefit from oral appliances before considering surgery.
Does insurance cover sleep apnea surgery?
Most insurance plans cover sleep apnea surgery when it's deemed medically necessary, typically after documented CPAP failure. Pre-authorization is usually required. Check with your provider for specific coverage details.
Can I use CPAP after surgery?
Yes. Many patients use CPAP temporarily after surgery while healing. Some may need to continue CPAP long-term if surgery doesn't fully resolve their OSA, though often at lower pressure settings.
Ready to Explore Your Options?
Connect with qualified sleep apnea surgeons to discuss whether surgery is right for you.
Find a Surgeon Near You